People with type 1 diabetes must take insulin and constantly monitor their blood sugar levels to avoid potentially dangerous fluctuations. A continuous glucose monitor (CGM) detects certain patterns to help your diabetes health care team adjust your self-management. While it does not replace standard blood glucose meters, a CGM can detect blood sugar lows that might otherwise go undetected.
- Recent research suggests CGM devices can help maintain good blood sugar control and minimize the long-term risks of diabetes while reducing the incidence of blood sugar events. According to a multi-center clinical trial done by the Juvenile Diabetes Research Foundation (JDRF), CGM devices make it possible for people to better manage their diabetes while reducing the frequency of low blood sugar, formally referred to as hypoglycemia. Typically these patients have already achieved excellent control (HbA1c levels below 7 percent) and want to minimize the possibility of low blood sugar emergencies.
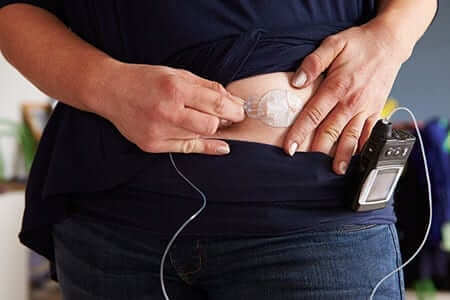
- A CGM system is an FDA-approved device that records blood sugar levels through the day and evening. A small sensor is quickly and painlessly inserted under the skin of your abdomen then secured with tape. Every 10 seconds, the sensor measures the glucose level in the tissue and sends the info through a wire to a cell phone-sized monitor. An average blood glucose level is recorded every five minutes for up to seven days before a new sensor is required.
- Beyond the automatic functions of the CGM system, patients should take a minimum of four finger stick blood sugar readings using a standard blood glucose meter then enter them into the CGM for calibration. Other activities are recorded in a paper journal then entered into the CGM including insulin taken, exercise done, and meals and snacks consumed. You simply push a button to mark the time of these daily events to be recorded.
- After the designated period, the CGM sensor is removed and replaced with a new one. The info stored in the monitor is downloaded into a computer. Graphs or charts are generated to show patterns of blood glucose fluctuations. This helps your diabetes health care team review these levels in relation to the other data collected and make adjustments as necessary to your current diabetes self-management plan.
- A CGM is not intended for long-term self-management or daily monitoring and does not replace the use of a standard blood glucose monitor. It is used to discover trends in your blood sugar levels to develop the most effective treatment plan for type 1 diabetes. A CGM can identify fluctuations that might otherwise go unnoticed with intermittent finger stick measurements and standard HbA1c tests. Examples might include morning spikes in blood sugar or low overnight blood glucose levels. This helps you more effectively manage your type 1 diabetes. Many private insurance carriers cover CGM devices and Medicare may offer reimbursement.
Talk to your health care team about whether using a CGM device is right for you. They can help you find out more about your blood sugar levels and certain trends that could impact your overall health. Consider using a CGM to develop a better diabetes self-management plan for optimum well-being.












Leave A Comment