What is continuous glucose monitoring?
CGM (continuous glucose monitoring) is an FDA-approved, user friendly system that measures blood glucose levels in “real time throughout the day and night.” By wearing a CGM you will have a better picture of what your blood sugars are doing from moment to moment. After initial calibration, the CGM measures blood glucose every 1-10 minutes. This make the CGM a “powerful and life changing piece of technology” for those with type 1 or 2 diabetes. It supplies the crucial information needed by you and your physician to make informed decisions about how your medications, exercise regimen and eating habits are affecting your diabetes management. Although, it may not completely replace standard glucose meters; it offers additional information by tracking trends. Informing you if your blood sugars are going up or down. CGM technology is changing rapidly and so is continuous glucose monitoring insurance coverage so stay informed.
What is in the CGM current research?
Recent research suggests that Continuous Glucose Monitoring can help maintain improved blood sugar control and minimize some of the long-term complications of diabetes. According to a multi-center clinical trial done by The Juvenile Diabetes Research Foundation (JDRF), “CGM devices make it possible for people to better manage their diabetes while reducing the frequency of low blood sugar.” Studies have shown that using a CGM “may help reduce your A1C levels up to 1% and can constantly identify trends in your blood sugars.
What does a CGM do?
- Reduces the risk of hypoglycemia and hyperglycemia
- Helps lower the 3-month A1C
- Improves the patient’s overall quality of life
- It helps reduce glycemic variability
- Increases “time spent in range” depending what your physician recommends usually between 80 mg/dl- pre meals and up to 180 mg/dl. 2 hours after meals
- It is especially useful for type 1 diabetes -patients on multiple insulin shots a day or on an insulin pump
- Is extremely helpful in special populations especially in hypoglycemic unawareness (experience no symptoms of low blood sugar)
- Patients hospitalized with diabetes especially difficult to control
How does a CGM work?
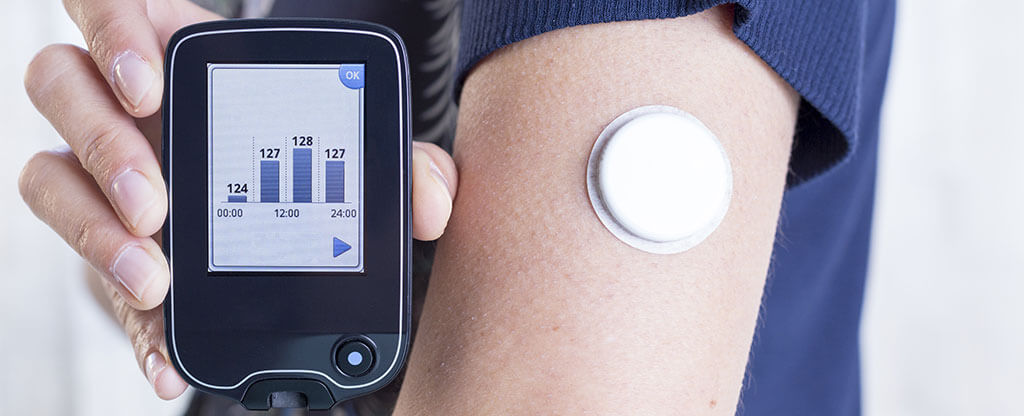
Place the sensor under the skin into the interstitial fluids, where glucose is found between the cells. It’s an easy and painless process since it’s tiny and flexible. The sensor is then secured with adhesive. Every 10 seconds the sensor measures the tissue level of glucose and sends the information to a receiver where you can view the readings. The average blood sugar is recorded every 1-10 minutes. The sensor may be worn on the abdomen or arm and stays in place for 3-14 days (depending on brand). Leaving the sensor in the skin for too long may cause skin irritation and scar tissue.
Moreover, the wireless transmitter that is attached to the sensor, sends information to a receiver which acts as a central system that displays the trends of your glucose levels. The receiver can wirelessly send this information to an insulin pump or Smartphone app when synced together. This gives you much more information than regular finger sticks because it tracks trends information onto a graph. Patients can set an alarm which alerts them when blood sugars are either too high or too low (depending on brand). Above all, blood sugar information in “real time” allows you to make informed decisions. Some CGM Devices send information straight to a second phone (parent, caretaker, spouse or health care professional) to provide immediate information about blood sugar trends.
Who should be using CGM?
- Originally recommended for patients with type 1 diabetes.
- Now recommended for those who take “intensive insulin therapy” or multiple shots daily, wear an insulin pump; either type 1 or type 2.
- Patients who can’t achieve A1C goals with regular fingerstick testing.
- With diabetes and can’t gain control somewhere between 80-160 mg/dl.
- It is excellent in identifying anyone with diabetes that is experiencing overnight lows and post meal highs.
- For patients unwilling or unable to count carbohydrates.
- Patients who are fearful of overnight lows.
- Women that are pregnant: pre, peri and post pregnancy
- People who have Gestational diabetes where diabetes appears only during pregnancy and may return years later.
- Patients and caregivers who want immediate real time feedback.
- Patients who experience the Dawn Phenomenon.
- If patients want to validate their proper medical treatment.
- Patients with diabetes who have eating disorders.
- Diabetes patients that want to be empowered with self-care.
- People frustrated or frightened of finger sticks.
- Children over the age of 2 with type 1 diabetes, when recommended by their physician.
- Patients who are extreme athletes or amateur athletes, who want real time blood sugar information before, during and after exercise.
Will I still need to do finger sticks with a meter?
Depending on the CGM you pick, will determine how many regular finger sticks you will need. To help your physician decide about possible changes to insulin dosages or medications; finger sticks may be necessary. Some CGMs do not require finger sticks for calibration. The Freestyle Libre and DEXCOM 6 do not require calibration finger sticks. Remember, to do a finger stick when symptoms do not match the numbers seen on the receiver/reader or if you have questions or concerns.
Who Covers Continuous Glucose Monitoring Systems?
Many insurance providers including Medicare may cover and offer reimbursement so find out from your insurance provider what your benefits are.
What are some options for CGM devices?
Always check the specific manufacturer’s manual for detailed information on the CGM you choose. Each one is slightly different and may require certain specific parts.
Medtronic Mini Med Guardian Link 3 transmitter Kit Features Include:
- Guardian Sensor 3 continuously monitors glucose levels when paired with the Guardian Link 3 transmitter and 670G insulin pump.
- Automatically adjusts basal insulin levels on your 670G pump.
- The Guardian Link 3 transmitter collects data from the sensor and sends the information wirelessly to the pump.
- Easy to insert into the subcutaneous layer of fat under the skin and can be worn for 7 days. It is a single use product.
- The only FDA approved sensor to control insulin dosing.
- It compliments not replaces standard blood glucose monitoring devices. Do not make treatment changes just based on CGM results.
- Worn on the abdomen [at least 2 inches away from the navel] or on the back of the upper arms.
- It is water resistant.
The Dexcom G6 is the newest generation CGM Features:
- It is the new and improved CGM G6 generation replacing the G5.
- It has an easy one button and one-handed applicator for sensor insertion.
- There is no need for finger stick calibration- calibrated at the factory.
- After insertion, there is a 2 hour warm up period- immediately begins real time CGM display.
- The slim transmitter sends data to a Smart device or the Dexcom 6 receiver. There are APPS for Apple and Android.
- Displays trends and patterns with a quick glance at your receiver or Smart device.
- Proven to help lower A1Cs and reduce hypoglycemic events.
- FDA approved
- Diabetes treatment without finger sticks.
- You can customize alerts and alarms.
Freestyle Libre by Abbott Diabetes Care Features:
- This is the latest CGM on the market. It is user friendly, easy to use and convenient.
- Scanning the sensor with the reader or smart device, is known as “flash” glucose monitoring.
- Only used in those 18 years of age and up.
- Factory calibrated, so no finger stick calibration is required.
- Place sensor in the subcutaneous fat with a one button application.
- The sensor can be worn up to 14 days. It can be scanned thru clothing.
- With each scan of glucose reading, you get 8 hours of current glucose reading and arrows pointing in the direction of where glucose is heading.
- Can be worn in the shower since is water resistant.
- Full 24-hour data can be captured and downloaded when the sensor is scanned at least every 8 hours.
- Never place where there can be bending of the body.
- Place sensor in approved areas like the upper back of the arms.
- Alarms are not provided for this CGM. Must scan sensor for 1 second for visual results.
Talk to your health care team to see if you can get better control of your blood glucose levels using a CGM device. Consider using a CGM to develop an improved diabetes self-management plan for optimal well-being. Know your choices.













Leave A Comment