Each year those of us in the diabetes world set aside November to help people with diabetes. We want them to become more aware of what they need to do to manage their disease. Keeping blood sugars controlled, preventing complications and making positive steps to live a full and healthy life are just a part of what we would like to accomplish. There are reliable web sites available to you including N.D.E.P. (National Diabetes Education Program) sponsored by the CDC which can guide you to make better daily decisions about your diabetes care. Working with your physician is imperative throughout the year to obtain excellent control. I wanted to share a look back at some of the moments in the history of diabetes and how far we have come.
- In 1500 BCE ancient Egyptians recognized diabetes in people who urinated frequently and lost weight for no apparent reason. It was not labeled at that time but it existed.
- A Greek physician named Arateaus recognized that the urine produced from people with diabetes was sweet and termed it Diabetes Mellitus.
- In 1776, Matthew Dobson actually measured the urine for glucose and found it to be increased in certain people.
- In the early 1800s diabetes was considered a clinical entity but the prevalence was not really documented. No specific treatment was used and usually within weeks to months the disease was fatal.
- The last 200 years have helped us understand many of the underlying causes of diabetes, ways to decrease risk factors of diabetes and actual treatments. The outlook has definitely improved with good results when therapies are used.
- Treatments have been effective but still no real cure has been made.
- The disease of ancient times involved insulin deficiency. (Type 1)
- In the early 1900s, Edward Sharpey-Schafer thought the lack of insulin was the cause of diabetes.
- Frederick Bating and Charles Best discovered insulin by reversing diabetes in dogs after inducing it. They did this by extracting pancreatic islet cells from healthy dogs; they later purified the insulin and along with James Collip and John Macleod were the first to treat a patient having diabetes with insulin.
- In 1936, Harold Himsworth proposed that more people had insulin resistance than insulin deficiency. (Type 2)
- The discovery of biosynthetic human insulin replaced animal insulin which eliminated reactions to insulin.
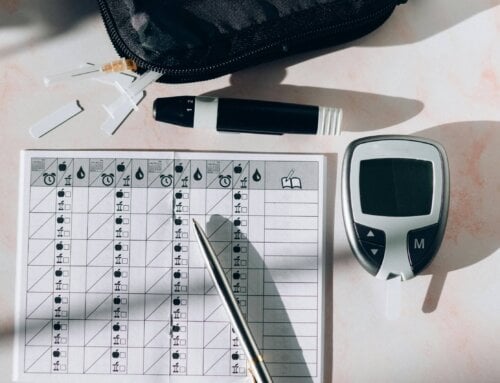
- Over the years we went from checking glucose in urine samples to using glucose meters and checking blood sugar. In the beginning, the blood glucose meter was only available in the hospital. They became smaller; more sophisticated and were available for home use.
- New kinds of oral diabetes medication classes have been discovered working on the pancreas, liver, muscle cells, gut hormones, kidneys. Some that remain are cheap and reliable, while others are gone due to excessive side effects.
- Insulin injections went from glass syringes and long needles which needed to be sterilized and reused to disposable syringes with short attached needles. Even easier are the disposable insulin pens which just require a click with a button.
- Pumps have made many lives much easier and eliminate the need for multiple daily shots. The added flexibility helps with an easier meal plan and exercise plan.
- Continuous Glucose Monitoring (CGM) assists people to identify blood sugar trends and is crucial for those who suffer from hypoglycemic unawareness.
- Ketone testing has gone from testing urine with strips to blood ketone testing with a meter which is more efficient and reliable.
- New injectable medications called GLP1s have been developed to not only assist with blood sugar control but with appetite suppression and weight management; a huge asset for people with diabetes.
- Bariatric surgery has been added as a treatment for extremely overweight people with diabetes. Good results have been seen.
- New technology and medications are always being developed since diabetes is big business. The future looks bright. Hopefully we will gain progress in the fight against diabetes.
- On the darker side, 2012 shows that insulin deficiency accounts for 10% of diagnosed cases (autoimmune), which can be controlled with exogenous insulin (Type 1). 90% of the cases are considered insulin resistance (Type 2). This has become evident in the past 40 years and has created an epidemic worldwide. (Inactivity, food portions and weight gain along with genetics-life style choices.)
- The most recent statistics from the ADA are: 26 million people in the US have diabetes; 79 million have pre-diabetes with an increased risk for diabetes. One in three will have diabetes in 2050 if dramatic changes are not achieved. The yearly cost of diabetes to the nation is $174 billion.
- The need for a team approach with multiple follow up appointments has proven results whether in person, one on one, class or on the phone. Having a physician, CDE, dietitian, social worker, podiatrist, pharmacist and ophthalmologist is the best way to follow all the organ systems involved in diabetes.
Unfortunately, even with all the advances in diabetes treatment from early times, the worldwide prevalence of diabetes just continues to grow. Knowing what to do to help our patients, and translating it into them actually doing it, still has some disconnected. The ability to treat diabetes in the future is likely to overwhelm the medical systems throughout the world if we do not figure this out.
This November, use Diabetes Month to get involved in a worthwhile cause. Learn to understand and help others understand what diabetes is, the frustrations it may bring and the joys of what feeling and doing better means. We have come far in our journey but we still have a long way to go in the fight against diabetes. Keep focused, get involved and stay informed!
NOTE: Consult your Doctor first to make sure my recommendations fit your special health needs.











Leave A Comment