Missed the previous article? Check it out here Back to Basics for Diabetic Pets | Part 1
Back to Basics Part 2: Pet Insulin
We are going back to some of the basic questions pet owners may have when they learn their beloved pets have diabetes. Today the topic is insulin.
What is Insulin?
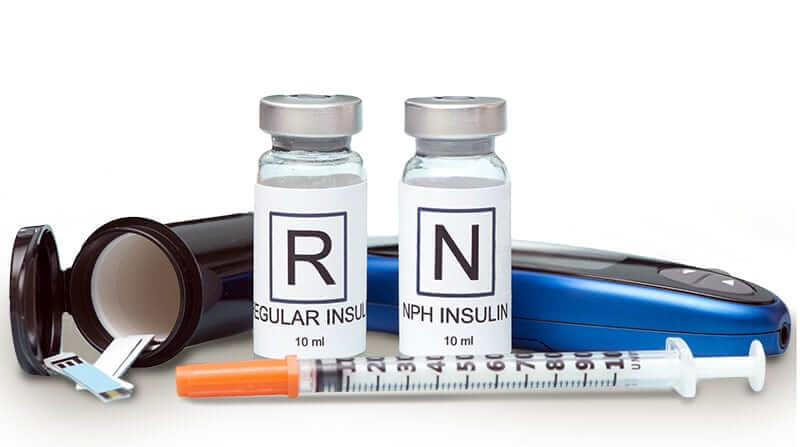
Insulin is a hormone made by the pancreas. It facilitates entry of blood glucose (the energy from the food we eat) into cells of the body. Without insulin we will starve, no matter how much food we eat. If a pet is not producing insulin, or if a pet is producing inadequate amounts of insulin, we can provide insulin for the pet by injections. Insulin injections are usually given to a diabetic pet twice daily, with meals. Sometimes we use insulin made specifically for pets. Sometimes we use insulin made for humans in pets. The most commonly used insulins used for dogs are Levemir, NPH and Vetsulin. The most commonly used insulins in cats are Glargine, PZI and Levemir.
What Does U-40 and U-100 Mean?
This goofy jargon refers to the concentration of insulin. U-40 means there are 40 units of insulin in one cc (cubic centimeter) of the solution. U-100 means there are 100 units of insulin in one cc of solution. One cubic centimeter equals one milliliter (ml). Knowing whether a particular insulin is U-40 versus U-100 matters because you need to be sure to buy the appropriate syringe for that type of insulin. I recommend NEVER using a u-40 syringe with u-100 insulin or vice versa. You can find calculators on the Internet for adjusting the volumes, but why bother? Math errors are killers. If you overdose or under-dose your pet, because the syringe type did not match the kind of insulin you are using, you will regret it. Just get the right kind of syringe for the right type of insulin. Math errors can be expensive and dangerous.
Suspending the Insulin
Insulin particles will settle to the bottom of the vial (or pen) when sitting in the refrigerator. It is important to evenly mix these particles into the fluid in the vial or pen before drawing up the solution to give to your pet. Don’t shake the insulin as that can damage the insulin particles. Instead, roll it between your hands or gently invert the insulin several times before using it. If you don’t do this the insulin at the start of the bottle will be less concentrated and the insulin when you get to the end of the bottle will be more concentrated. That could wreak havoc on diabetes control!
Rotating the Injection Sites
When I first teach pet owners how to give an insulin injection they often have a “deer in the headlights” look about them. Asking a pet owner to poke their beloved pet is daunting for many people, no matter how teeny tiny the insulin needle may be. For this very reason, I have diabetic pet owners start giving injections in the scruff of the pet’s neck and shoulder area. We start up in the scruff because it hurts less in the scruff.
Once a pet owner gets confident with giving injections I have them start moving the injection sites around. Why? If you repeatedly give the injection in the same site it can form scar tissue which may hinder the absorption of the insulin over time. Another important yet often forgotten tip is to rub the injection site before, during, and after the injection. Rubbing the skin will stimulate the nerve receptors in the skin and decrease discomfort. Remember how your mom likely said “rub it to make it feel better” when you were a kid with a boo-boo? Mother knows best!
Please Refrigerate the Insulin!
Yes, I know that humans often leave their insulin outside the fridge. Some say it hurts less when it is room temperature than when cold from the fridge. Humans usually need a larger volume of insulin than our little veterinary critters require. Nonetheless, refrigeration prolongs the shelf life. Germs don’t grow as well in a cold environment as in a warm environment. To be honest, I can’t recall a pet reacting to an insulin injection. Of course I rub the injection site and the volume we administer to dogs and cats is pretty small. Whether that itty bitty volume is cold probably doesn’t make much difference in sensation to a pet. Keep the insulin in the fridge. Additionally, always monitor the insulin for discoloration or cloudiness. If it looks at all different, toss it and start a new vial.
How Often Should You Change the Vial of Insulin?
Boy is that the million dollar question! On the vial or pen of any insulin it will say one month. Let me tell you, I hear a lot of grumbling about that from pet owners. Pets (especially small pets) don’t use but a fraction of a vial in one month. If finances are a concern, I let my clients use a vial for 2 months provided they adhere to strict hygiene. My usual joke is that I don’t want it rolling around in the butter dish in the fridge! I recommend leaving the vial in the box and make sure nothing but a fresh insulin syringe touches the rubber top. Additionally, whenever possible, I like my clients to use pens when they are available. Pens only have 3cc of insulin compared to vials which have 10cc of insulin. There is so much less waste when using pens. Less waste means less costs to pet owners. Lower costs mean less grumbling at veterinarians about the cost of Fluffy’s vet bills. Diabetes ain’t cheap, so be smart when buying your insulin. Many pens don’t allow for half doses, so fine tuning a dose doesn’t work well with the pen needles.
Instead of Insulin Injections Can I Use an Oral Hypoglycemic Agent Like Glipizide?
Doesn’t this sound tempting! Most folks would rather give their beloved pet a medication by mouth rather than an injection. Unfortunately, dogs are type 1 diabetics (aka insulin dependent diabetics). Oral hypoglycemic agents like glipizide are for type 2 diabetics. Cats are usually type 2 diabetics (at least when initially diagnosed), so vets have tried using oral hypoglycemic agents for cats. I would not recommend this because our goal with newly diagnosed cats is to reverse glucose toxicity and get them into diabetic remission. Diabetic remission rates are much higher in cats on insulin and canned low carb diets than with other treatment protocols. If we waste precious time using oral hypoglycemic agents (rather than starting insulin and using a low carb diet) we may never get a cat into remission. The type 2 diabetes may turn into insulin dependent diabetes.
Next week the topic is blood glucose monitoring and diabetes assessment. Check out Back to Basics for Diabetic Pets | Part 3
Have a question or comment? Post below or email me at [email protected]. I always enjoy hearing from my readers!
NOTE: Consult your veterinarian first to make sure my recommendations fit your pets special health needs.












Something that my vets did not tell me and that I found out by accident is that Walmart carries a house (Reli-on) brand of Novolin N (good for 42 days after opening, U-100) that is only $25 a vial (10cc). It is exactly the same thing as the brand version. After spending $130 a month for the same thing at the grocery store pharmacy several times, finding this out was a godsend. Also Walmart syringes (u-100) are much cheaper than at the grocery store or drug store and they always have the 29G 1/2 inch syringes I need, unlike the grocery store.
Yes, it is a really good deal at Walmart. Thanks for sharing! Most folks don’t see much difference between novolin N and humilin N for their pets, but some readers have told me they needed to alter the dose a bit up or down when making the switch between these insulins. I asked my own home town pharmacist a few years ago why there was a cost difference between these 2 NPH insulins and he had no good explanation for me!
At least with regard to the Reli-on Novolin N, I think it is a testament to the purchasing power of Walmart. I also wanted to say, due to my Westie’s brittle diabetes, I must test him prior to each insulin injection and do curves when we lose control, and he does not mind the testing. I use the ear area. Even though he has been hard to control, he is almost a year and a half since diagnosis and still no cataracts, I believe because we have tested him frequently and worked hard to keep him regulated. Thanks for your response, and thanks for the column, which I really enjoy.
Janey, speaking of eye health, do consider ocu-glo to help lent the diabetic cataracts. It contains alpha lipoid acid and other good eye hewtlthy vitamins and antioxidants and has shown to delay the onset of diabetic cataracts. It’s a great supplement made by a vet ophthalmologist. They have proof it works. We carry it he at ADW. 🙂
Is it ok to feed brown rice to my dog that has diabetes?
Brown rice is fine. I’d avoid white rice. And of course brown rice would be at mealtime as portion of the meal. Mid meal snacks aren’t recommended as food at a time other than when insulin is given could cause an unwanted blood glucose elevation.