When veterinarians do diagnostic testing to diagnose diabetes, the tests we suggest may seem confusing to pet owners. I assure you they are not. Let’s discuss some commonly recommended tests for diabetic pets and how often and when we may run them! Let’s start with discussing tests for the pancreas, the organ that makes insulin. Then, we will discuss blood glucose tests and chemistry profiles. And finally, we will discuss various urine tests.
The Pancreas and Diagnostic Testing of the Pancreatic Function
The pancreas is an amazing organ. It makes the hormone insulin which facilitates the utilization of energy (glucose) into cells. Without insulin we see the clinical signs that my readers know all too well: excessive thirst, urination, hunger, weight loss, etc. A lack of insulin is known as diabetes mellitus. The pet may have complete loss of insulin production. Or, it may just be a relative insufficiency of insulin. Regardless, we start the pet on insulin injections at the time of diagnosis and adjust insulin dosing as needed by testing blood glucose levels.
Sometimes a pet still has the ability to make some insulin, and if we get rid of common causes and factors leading to insulin resistance (such as obesity, infection, high carb diets and steroid use) we may get a pet into diabetes remission and can stop the insulin injections. Remission is most common in cats and only rarely blesses us in dogs. Newly diagnosed diabetic cats may be experiencing what is known as “glucose toxicity”, which means that the beta cells in the pancreas are inhibited from producing insulin when the blood glucose is elevated. Dogs may also experience insulin resistance and glucose toxicity, but typically once a dog is a diabetic it will remain diabetic. The notable exception is gestational diabetes secondary to progesterone influence in an intact female dog when she is in season or pregnant.
We don’t typically measure insulin levels in pets unless we are concerned about an insulinoma. An insulinoma is a tumor of the pancreas that produces insulin. If a pet has an insulinoma the pet makes too much insulin, pretty much the opposite of diabetes. Insulinomas are rare and result in very low blood glucose levels. I only mention this because some of you will wonder why we don’t measure insulin levels for diabetic pets. Rather, we concentrate our efforts on measuring blood glucose levels instead of insulin levels. We will discuss blood glucose levels later in this article.
The pancreas also has a digestive function. Now, what happens if the pancreas doesn’t produce the enzymes to digest fats? This situation is called exocrine pancreatic insufficiency. EPI pets tend to be quite thin and have chronic loose stool. Luckily, this disease isn’t particularly common. I have one patient with this disease. He is a German shepherd and does great so long as we give him pancreatic enzymes in his food. He came into my clinic quite lean and with a history of soft poop. We tested him last year with a blood test called a TLI then added the pancreatic enzymes. He now has great body condition and nicely formed poop. Every day the owner incubates his food with the enzymes for 20 minutes before feeding him.

Pancreatitis can result in an injured pancreas that may then not produce insulin (the hormonal function of the pancreas). As many diabetic pets become diabetic following a battle with pancreatitis, we typically encourage a low fat diet for diabetic pets whether they are dogs or cats.
Now, how do we diagnose pancreatitis? There are actually several tests that may clue us into pancreatic inflammation. On a full chemistry profile there are several pancreatic enzymes listed. Amylase and lipase are the enzymes usually listed on the profile, but in recent years there have been improvements in the lipase tests. Idexx is a diagnostic lab that came out with new tests called a Spec cPL for dogs and Spec fPL for cats a few years back. They test for lipase specifically from the pancreas rather than the total serum lipase on the typical blood panel. This test is fantastic. And yet, sometimes these tests fail us. We may also diagnose pancreatitis using diagnostic imaging, usually ultrasound. If a diabetic pet isn’t eating well, we should be on the lookout for pancreatitis.
Blood Glucose, Glucose Curves, A1A and Fructosamine
If we run a blood profile and identify diabetes mellitus, we will start a pet in insulin. Unfortunately, that’s not the end of the story. Wouldn’t it be fantastic if every diabetic pet had perfect blood glucose regulation just by starting insulin injections? Alas, that is a fairy tale. Earlier in this article, I told you that some diabetic pets may still be able to make some insulin? It could be a relative insulin insufficiency that we are treating rather than a complete insulin deficiency. The amounts of insulin a pet can make or will need may change over time. Some pets may need more insulin than others. Insulin requirements also depend upon the amount and type of food ingested. Some pets absorb insulin better than other pets. Some pets metabolize insulin more quickly than other pets. No two diabetic pets are the same. So we are left monitoring the blood glucose to see how well we are regulating the pet’s blood glucose control.
When I graduated vet school a quarter century ago, we routinely had diabetic pets spend the day in the hospital for blood glucose curves. A curve means we check the blood glucose every 2 hours from one insulin injection until the next insulin injection 12 hours later. A curve tells us how low the blood glucose goes. This number (where it bottoms out) is called the nadir of the curve. We don’t actually have to plot out the curve on a graph. In fact, I never do. I do, however, ask folks to check the blood glucose hourly when/if the blood glucose goes below 150 mg/dL until the level starts to rise again. This way I don’t miss the nadir. The nadir is important because it is the number that tells us if we should increase the insulin dose or decrease the insulin dose or leave it where it is. We like the nadir to be somewhere around 100 mg/dL.
What else does a curve tell us? It tells us how long the insulin lasts in a pet. Ideally an insulin will last 12 hours as we typically give pets insulin injections every 12 hours. If the blood glucose rises after 5 or 6 hours and we have very high glucose levels for the back half of the injection period, the pet may show the clinical signs we wish to avoid. Excessive thirst and hunger and urination aren’t fun for anyone! I imagine the pet is uncomfortable and/or frustrated and the pet owner is left frustrated and worried. If a pet’s nadir is perfect but the insulin doesn’t last long enough, we may need to change to a longer acting insulin.

In the last 10 to 15 years, home glucose testing has become the norm. I’m so glad. There are now several pet glucose meters on the market. I do strongly prefer using a pet glucose meter over a human blood glucose meter as human meters tend to underestimate the blood glucose of pets.
Now, what if your pet is non-compliant at the vet office. Every now and then I’ll have a client who is physically incapable of checking a blood glucose on the diabetic pet. If the pet is friendly and not terribly stressed at the vet clinic, we will run a blood glucose curve at the clinic. Again, I fear the stress of the clinic will cause stress hyperglycemia but now and then I’ll run a curve in the clinic. If, however, the pet is so stressed or naughty that a curve in the clinic is clearly causing stress I may instead forego a curve and instead run an A1c test (or in the past I would run a fructosamine test). An A1c test reflects back the prior 70 days for a cat and the prior 110 days for a dog. A fructosamine test reflects back the prior few weeks for dogs and cats. A1c and Fructosamine tests don’t give us the same information as a curve, but sometimes we must settle for the information that we can get.
Urinalysis, Urine Dipstick, Urine Sediment, and Urine Culture
I’ve been practicing veterinary medicine since 1993. I’ve seen a dramatic shift in how we manage diabetic pets in that time. Many years ago, we would have clients use urine dipsticks to help assess glucose regulation of their diabetic pets. We’d tell them that we didn’t want it to always be negative and we didn’t the test strips to always come up as strong positives for urine glucose. And we’d run a blood glucose curve in the clinic periodically. Boy have times changed! Now those suggestions seem horribly outdated and crude.
These days we rarely have clients check urine dipsticks for to assess glucose regulation. As I wrote earlier, we now have great pet glucose meters. And there are lots of videos and blogs like mine. The internet has helped veterinarians teach folks how to check blood glucose levels at home with little lancets and pet glucose meters. We are light years ahead of where we were just a few decades ago.
The glucose threshold for dogs and cats is somewhere between 250 and 300 mg/dL. For example, if the blood glucose is at 225 mg/dL at some point in time the pet still has diabetes, but won’t be spilling sugar into the urine at that blood glucose level. The pet still is diabetic and needs help utilizing the energy from the food it eats (via insulin injections for the pet owner), but it won’t be peeing excessively when the blood glucose is 225. Clearly the blood glucose changes throughout the day for a diabetic pet. Likely there will be glucose in the pee at times and no glucose in the pee at other times. A diabetic pet won’t be excessively urinating until the blood glucose hits 250 or 300 mg/dL. It is when the pet pees excessively that it then needs to drink excessively just to stay hydrated.
If you understand this bit about the glucose threshold in the kidneys, you will understand why it’s ideal to have most of the blood glucose values under 300 mg/dL. If we manage to keep the sugar levels under 300 mg/dL, most diabetic pets won’t be excessively peeing and drinking. I think it must be frustrating for pets to constantly need to go potty and to constantly be thirsty. The quality of life is better when the pets isn’t polyuric and polydipsic! Thus, my ideal blood glucose curve will have most of the numbers under 300 and to bottom out around 100. If we could have consistently normal blood glucose numbers that’s even better.
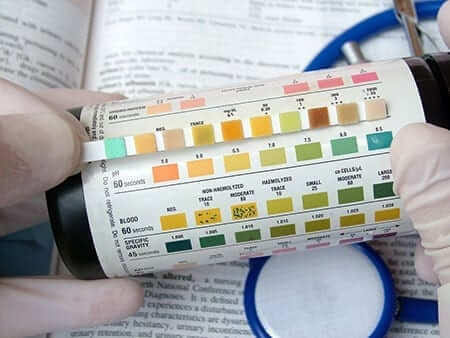
When might a diabetic pet owner use a urine dipstick? If your diabetic pet is fragile and has been in ketosis (a negative energy state when the diabetes isn’t controlled), you might consider checking urine dipsticks now and then, especially if your pet isn’t feeling well. If you are physically unable to check blood glucose levels for your diabetic cat and think your cat might be nearing diabetes remission, you might periodically check urine dipsticks (to see if the glucose levels come up negative frequently).
We often recommend a urinalysis several times per year for diabetic pets. Even better is to check a urine culture for a diabetic pet. Imagine that you were a bacteria. What nicer place than a bladder full of sugary pee could you find to cause an infection! Since many diabetics have elevated blood glucose (that exceeds the kidney glucose threshold) it’s is also often dilute urine simply because of osmosis. It may be hard to identify an infection in dilute urine because the cells and bacteria are less concentrated. Therefore, we take some urine and submit it to the laboratory for culture of bacteria. This urine must be collected aseptically, usually by pulling it from the urinary bladder via a needle.
Urine cultures can be pricey! I pay my local lab nearly a hundred dollars for urine culture and sensitivity testing. I submit these tests when I think there is a doozy of a bladder infection. However, I also own a urine incubator in my vet clinic. I often start urine cultures in my own clinic for significantly less money. I’m not a clinical pathologist nor a microbiologist, but a negative is a negative and my in house urine cultures are a heck of a lot less expensive than a negative at the outside reference lab. If something grows in the in house culture I can submit it to the outside lab to check it’s sensitivity to various antibiotics. If the culture is negative, I saved the owners a bunch of money. I typically run a urine culture on my diabetic pet patients at least twice yearly, even when the urinalysis is unremarkable.
Have a question or comment? Then post below! I always enjoy hearing from my readers!
NOTE: Consult your veterinarian first to make sure my recommendations fit your pets special health needs.













Hi Dr. Joi. I have a question about diabetes and Cushing disease. My 13 year old toy poodle has been diabetic for 3 1/2 years. He was tested for Cushing disease at the onset of his diabetes, but Cushing was ruled out. Is it possible for him to get Cushing disease now after 3 1/2 years?
It is possible to get Cushings even if you are diabetic. Typically we think of the Cushings causing diabetes, but they can co-exist. Your vet can run some tests again to find out. 🙂
I have a cat that was diagnosed as diabetic in September 2017. He seems to be doing absolutely wonderful! He has regained the use of his hind legs, and is back to being his old self. He is running, jumping up again to high places. His last blood glucose reading was117mg/dl. I need to understand remission. I cannot find a clear explanation regarding it.
My vet is very vague, and says he has not seen by one cat go into remission. I have just received a blood monitoring kit from your site. I will be doing that testing here at home, but will keep in contact with the vet. Please explain remission, what do I look for? What do I do? Thank you so very much!
Hi! I’m so glad for you! This looks promising. I actually write an article on this very topic a couple years ago. You can simply type the title into the articles search box on our website.
Great job!
What to Expect When Your Cat Goes into Diabetic Remission
Posted by Dr . Joi Sutton | Sep 11, 2014
I have both a cat and dog with diabetes and on insulin. I purchase the prescription foods from my vet and on reading the contents of the foods , I see corn, corn gluten, soy, chicken or liver flavoring and other fillers. Looking at better pet foods, such as Earthborn Holistic, which has protein meals, veggies, fruits, omega 3 and 6 and no fillers, I wonder why I have to feed my dog and cat food my vet says is needed! They say the prescription food is certified! I really don’t like feeding my pets food with corn, soy or wheat,. I understand carbs and proteins myself, but veggies and fruit have the carbs. Being a type 1 diabetic myself, I just don’t understand this! Help, please. Thank you.
The primary goal with a diabetic cat is to feed a diet low in carbs. For dogs, we want low glycemic high fiber carbs. For both diabetic dogs and cats we want low fat diets as many diabetic pets are diabetic followi an episode of pancreatitis. (Fatty foods can exacerbate pancreatitis.). If you wish to do home cooked diets, this would be great! Most folks aren’t willing or able to make their diabetic pet’s foods. You don’t need to feed “prescription” food, but it may help as nutritionists formulate the diets/ingredients.
🙂 Joi
Great info, thanks so much for your efforts. Especially about pancreatitis and keeping the #s < 250. I tend to over worry about lower #s, so I guess we're doing ok!
We have a cat who has been diabetic for about 6m years. Fortunately the cat is very compliant and giving blood glucose checks and injecting is easy. I have a question:
1) How long would a cat have to have a blood glucose over 300 for organ damage to occur? A few days? A week? a month? I get a high reading maybe once a week. It can be 500 to 600. Is this infrequent high harmful in the long term? Does any damage accumulate or does any damage mend after the glucose level is again in the below-300 range?
I suspect the reason for these occasional high readings has top do with the injection itself. The cat has a loose skin so when I make the “tent” both sides come together and it is hard to locate a hollow place under the skin.
Thanks,
Kurt Buermann
Sharon, MA
Kurt, I don’t think actual data exists to answer you accurately. Clearly, the better the control the better the long term quality of life and less the chances of a crisis. Do you run blood glucose curves at home? Do you feed canned, low carb food only to your cat? Those 2 simple things can improve the diabetic control dramatically for your kitty! 🙂 Joi