Managing diabetes is an ongoing challenge as people try to keep their blood glucose levels stable. Knowledge and the right equipment can make a major difference. Discover a few diabetes devices to help make your diabetes life easier.
The I-Port Takes Shots for People with Diabetes
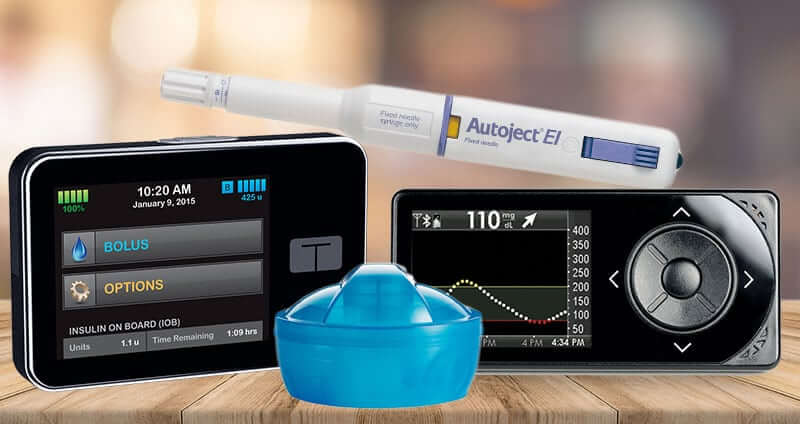
Many people with diabetes need to administer insulin throughout the day. With the I-Port injection port, medications can be taken without the need to puncture the skin for every shot.
Ease of Use for Regular Injections without the Pain
This device can be worn for up to three days. People can continue to engage in normal activities while wearing it, such as exercising and showering. An American Association of Diabetes Educators (AADE) survey revealed nearly half of people would administer essential injections regularly if a product could ease the discomfort. Unfortunately, these people also skip injections because of the fear of pain. The I-Port may decrease the stress associated with each injection by reducing the number of times the skin must be punctured. A built-in inserter device inserts the device quickly and painlessly. A cannula, which is a flexible tube measuring 6 mm or 9 mm, stays under the skin. This is where medication is injected through the device by using a standard insulin pen or syringe. However, the needle does not touch the user’s skin.
Discreet Insulin Administration with Insulin Pens
People with diabetes can streamline the administration of insulin by using insulin pens. The injections are discreet because the insulin and injection device are one simple unit and are very portable.
Simplicity is Convenient
With insulin pens, people no longer need to carry separate insulin vials to draw medication into the syringe. Some insulin pens are reusable and get refilled by using disposable insulin cartridges. Others insulin pens are disposable and come pre-filled with the specific type of insulin required. Once empty the pen can be thrown away. Different brands and types of insulin can be administered through insulin pens. This includes bolus (rapid acting) insulin and basal (long-acting) insulin. Some are filled with blends, based on the patient’s needs. The disposable pens are color-coded to ensure the patient administers the right type of insulin. Consider dating the pen when opened and follow the manufacturers suggestion for how long the pen can be used once opened. Pens are excellent for those with low vision since they make an audible click with each unit dialed up. Dosing is a consideration when using insulin pens. Some come with whole units, others with half units. The needles should be removed after each injection and a new sterile needle needs to be replaced with each following injection. Learn to dispose of needles properly by contacting your health department.
Patients Get Control with Autoject
Autoject is an automated injection device to help patients get more control over administration of medication. The device helps to make the process more manageable.
Concealment for Injections
Some people with diabetes are anxious about injecting themselves. The Autoject conceals the needle and syringe to minimize stress and protect the patient against accidental injuries. The patient simply touches a button to administer insulin. This is an advantage for elderly people and children who might find it challenging to administer injections. The one-handed operation makes it possible to use a wider variety of approved injection sites. Visual and audible indicators mark the start and end of injections to administer medication accurately. Errors are minimized with a safety mechanism that prevents firing until the device is pressed against the patient’s skin. Injections can be tailored by using the needle depth adjuster. The Autoject can be used with various syringes.
Insulin Pumps to Manage Diabetes
The need to constantly manage diabetes can become stressful for many people. An insulin pump makes it easier to maintain control over blood sugar levels while handling the other demands of daily life. About 20 percent of people with diabetes use one. Most insulin pumps are used by people who have diabetes type 1 but some health insurance policies may cover type 2 as well. It eliminates the need for multiple daily injections by putting a catheter/cannula into the body for 3 days. The cannula remains and delivers the insulin when the pump settings are activated. Pump training is offered by the manufactures of the pumps and should always be requested. Learning to use the pump correctly along with carbohydrate counting is crucial for diabetes control.
A More Carefree Lifestyle
Patients typically match their lifestyle to how the insulin they inject throughout the day is working. The goal to keep blood glucose levels within the target range of generally 80-150mg/dl. A pump helps keep blood sugars within range without constantly administering injections. Different amounts of basal and bolus doses are delivered during the day and evening. The amounts are established by an endocrinologist, a diabetes educator and/or a diabetes dietitian along with self knowledge from the patient. When a patient eats, a button on the pump is used to deliver more bolus insulin to cover the carbohydrate in the snack or meal. The pump can be attached to the person’s waistband, bra, underwear, or other convenient areas where the tubing can also be tucked in. Some pumps are now tube free. Though the pumps are water resistant, they should be disconnected when the person is showering or swimming.
Using a Diabetes Device CGM System for Greater Control
Glucose monitoring is necessary for people with diabetes to ensure their blood glucose levels are in the proper target range. A blood glucose meter or continuous glucose monitoring (CGM) system can be used to help people manage diabetes especially when they suffer from frequent highs and lows. A CGM constantly measures glucose levels to help people with diabetes get greater control by showing trends.
Measuring Blood Sugar Levels in Real-Time
When using a CGM, a tiny electrode (glucose sensor) is inserted under the skin to measure the blood sugar levels in the person’s interstitial fluid. The electrode is connected to a transmitter that sends the information to the monitoring device. The info is displayed and notifications are sent if the person’s blood glucose levels get too high or low. CGM systems need to be calibrated for the highest level of accuracy. This requires the use of a finger stick to calibrate the electrode. While a meter just provides a brief snapshot, a CGM shows ongoing blood glucose trends, including when a person is eating, exercising, sleeping, ill, and taking medication. This information can provide important information to improve diabetes management. Your health care team may decide to adjust medication and activities based on these ongoing results. Using a CGM can also help patients better manage their A1C levels and reduce the risk of hypoglycemia. Studies reported by the National Center for Biotechnology Information (NCBI) reveal CGM is an essential tool for effective modern diabetes therapy. It is often used in combination with an insulin pump.
Using Disposable Pen Needles
Disposable pen needles are sold separately from insulin pens and patients need a prescription to get them. The needle is snapped or screwed onto the tip of the pen. Needles come in different sizes and requesting the shortest ones may help reduce pain. Fresh needles also help reduce pain since they are sharp[dull reused needles cause more pain] and reduce infection rates.
Changing Needles after Injections
Disposable pen needles should be removed after each injection. Some pens have a built-in remover, and others have a needle shield that locks in after the injection to reduce finger sticks. The pen needles come in various lengths for all body types including 4, 5, 6, 8, and 12.7 millimeters. Thickness also determines the feeling of pain. The higher the needle gauge, the thinner the needle is. Typical gauges are between 29 and 32. Those who take larger doses of insulin may need to use a thicker needle for faster delivery and to avoid leakage.
Portion Plates for a Healthier Diet
A well-balanced diet is also important for good diabetes management. Sometimes it can be difficult to determine how much to eat from each food group during meals. Portion plates make it easier for people to find the ideal balance.
Visual Control over Diabetes Eating

Diabetes can be an ongoing challenge to manage but the savvy use of certain diabetes devices makes it easier. Discuss diabetes devices with your health care team to find ways to improve your diabetes management program. Plus, these devices can help you lead a healthier, more carefree life!












Leave A Comment